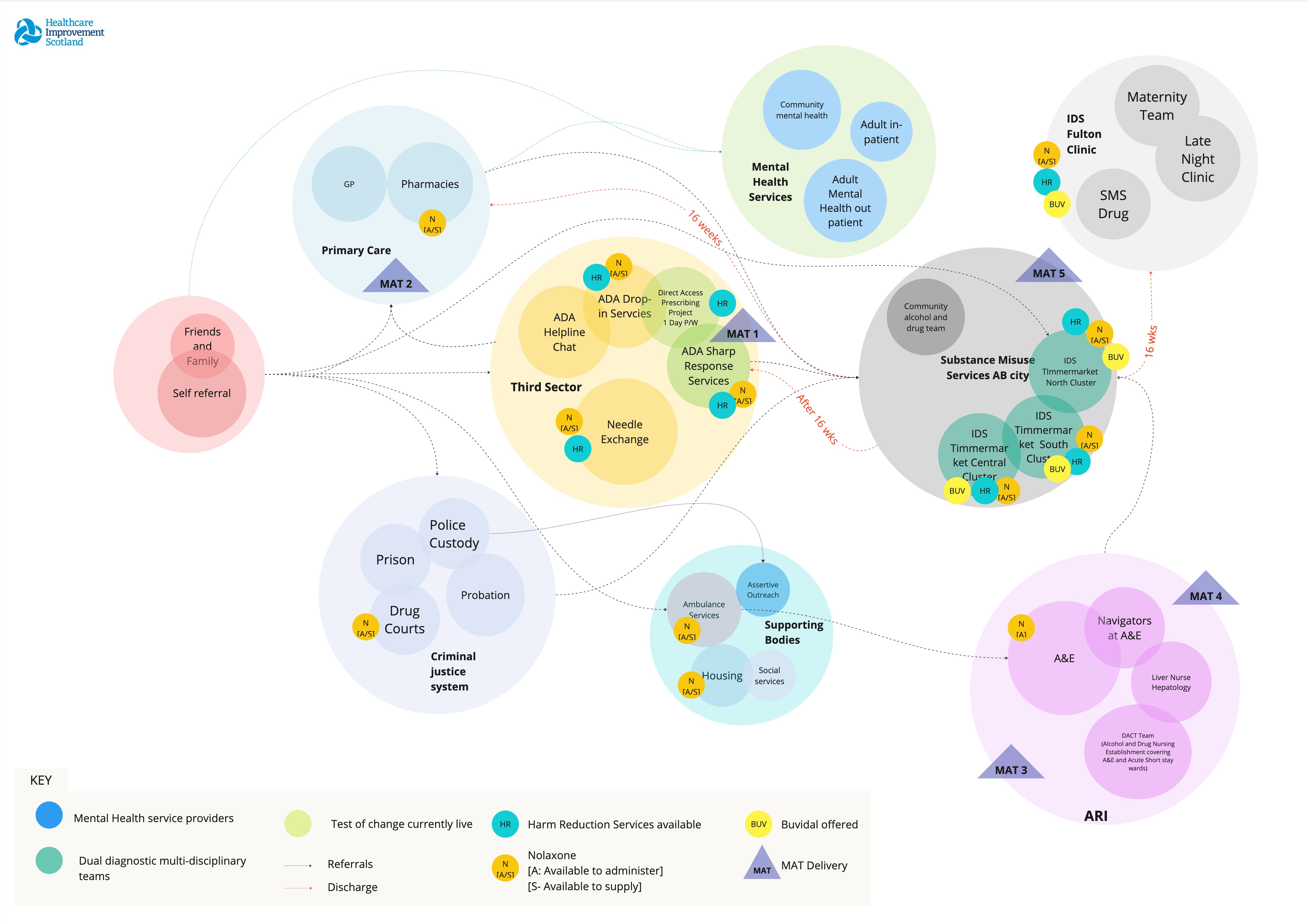
Using system maps to understand the complexity of Mental Health and Substance Use Services
We used system maps to understand the current service landscape and design a joint referral pathway for those with co-occurring needs for mental health and substance use (MHSU). This required understanding different organisations and their services offerings as well as their interconnectedness.
How we approached mapping:
- A crude map of existing mental health and substance use services was provided by one of the NHS boards at MHSU pathfinder sites.
- Service designers re-visualised the crude map facilitating a holistic view of the system and offering a tangible output aiding teams in structuring service needs and communicating the system comprehensively.
- Service designers used the system map for information processing, sharing, and learning as projects evolve through the identification of gaps, highlighting complexity, and revealing opportunities for targeted service interventions.
Using system maps enabled us to achieve the following
- Facilitating Knowledge Integration: System maps, when used as boundary objects, served as interfaces for knowledge integration, especially from clinical groups.
- Zoom in and out: Zoomed-out overviews allowed to focus on areas requiring detailed examination for joint pathway design.
- Focused Discussions: System maps provided a more focused discussion, clarifying service areas, their purposes, and interconnections.
- Reflective Tool: Used as a reflective tool for teams when developing specific service interventions.
- Bridging Function: Acted as a bridging function between clinical and nonclinical groups, facilitating communication and collaboration.
- Shared Understanding: Enabled teams to create a shared understanding of the system, enhancing decision-making and learning opportunities.